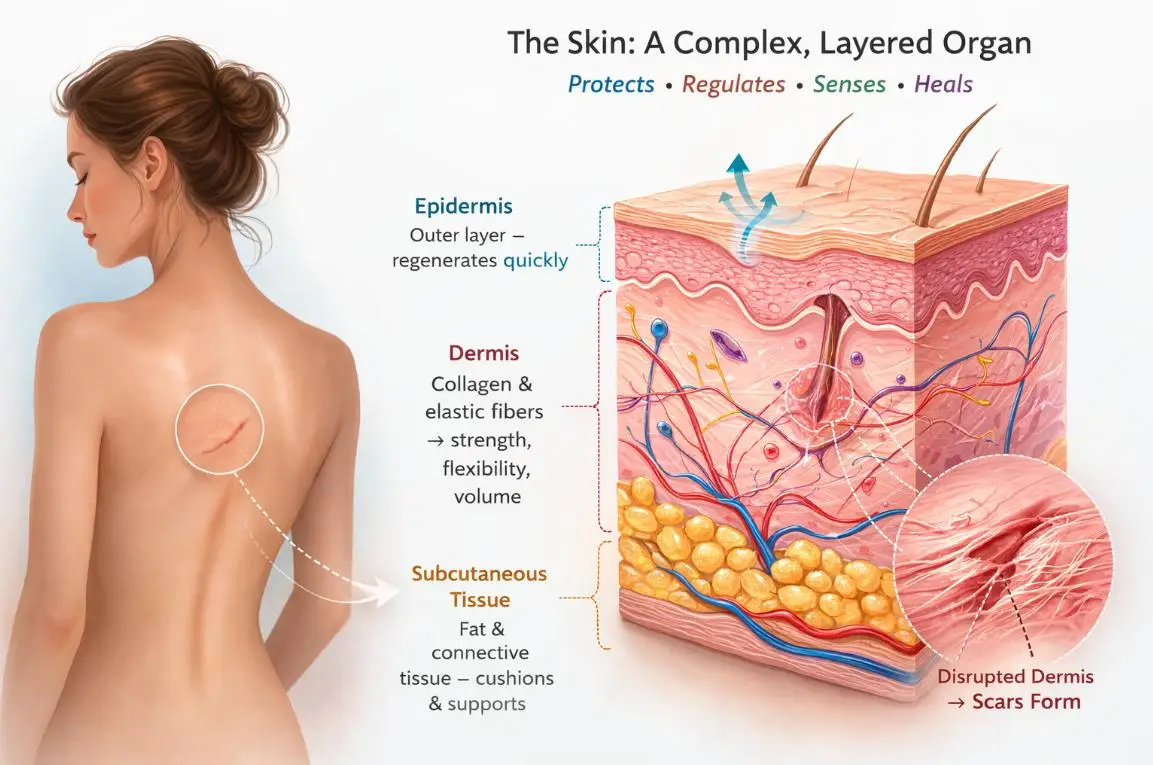
Our skin is more than just a covering; it’s a complex, layered organ that protects us, regulates temperature, senses the environment, and heals when injured. Yet, despite its remarkable abilities, the skin’s healing process often leaves behind scars — visible reminders of past wounds.
A Quick Tour of Skin Structure
Skin has three main layers:
- Epidermis – the thin, outer layer that acts as a barrier. It regenerates quickly after minor injuries.
- Dermis – a thicker, structural layer underneath, made of collagen and elastic fibers. This layer gives skin strength, flexibility, and volume.
- Subcutaneous tissue – a layer of fat and connective tissue below the dermis that cushions and supports the skin.
The dermis is especially important when it comes to scars: loss or disruption of dermal tissue often determines whether a scar will be flat, raised, or depressed.
How Scars Form
When the skin is injured, the body triggers a healing cascade:
- Clotting and inflammation stop bleeding and clear debris.
- Fibroblasts and other cells migrate to the wound, laying down collagen and extracellular matrix.
- The tissue gradually remodels, replacing early granulation tissue with stronger, mature collagen.
The outcome depends heavily on dermal volume, collagen alignment, and mechanical forces in the surrounding tissue:
- Flat scars occur when healing restores near-normal dermal thickness.
- Raised scars (hypertrophic or keloid) result from excessive collagen deposition.
- Depressed scars (atrophic, “crater” scars) form when the dermis is lost or underfilled during healing.
Why Some Scars Persist
Interestingly, two injuries of similar depth may heal very differently:
- A deep punch wound can heal perfectly flat if granulation tissue fills the defect adequately.
- A chickenpox crater, on the other hand, often leaves a persistent depression.
This observation highlights that dermal loss alone doesn’t explain everything. Factors like inflammation, ECM destruction, local tissue tension, and the organization of collagen bundles all play a role.
Researchers are still exploring why some scars seem to “persist” even when surrounding skin looks healthy. Conventional hypotheses include:
- Mechanical memory: the tissue around the scar may guide collagen deposition along certain lines.
- Fibroblast positional identity: cells remember where they are in the body and what type of dermis to form.
- Epigenetic programming: scars may leave chemical marks that influence healing.
None of these are definitive, and many scientists emphasize that much about scar persistence remains unknown.
Traditional Scar Treatment
For deep or crater scars, the standard approach is surgical excision with closure:
- The old scar is removed with a punch or scalpel.
- The edges are brought together with sutures.
- The new scar is often smaller, flatter, and more cosmetically favorable.
For deeper defects, sutured closure produces cleaner, more reliable results.
Emerging Approaches in Scar Healing
The cutting edge of research explores ways to actively guide tissue regeneration rather than simply excising scars:
- Electrical stimulation: Low-intensity DC or microcurrent therapy can direct cell migration (galvanotaxis), promote fibroblast activity, and enhance angiogenesis. By guiding cells into a wound, it may improve dermal filling and flatten depressed scars.
- Mechanical remodeling: Techniques like subcision or tension-controlled closure influence collagen deposition and scar shape.
- Tissue scaffolds and growth factors: These can provide a framework for cells to rebuild dermal volume more effectively.
While many of these strategies are still in research or clinical trials, they hint at a future where scars may not just be minimized, but actively regenerated into normal-looking skin.
The Takeaway
Skin is remarkable, but healing is a complex balancing act that we currently don’t fully understand. Whether a scar is flat, raised, or depressed depends on a combination of tissue volume, cellular behavior, collagen organization, and mechanical forces.
Modern science is now uncovering ways to guide these processes, from careful surgical techniques to electrical stimulation and regenerative scaffolds. Though we don’t fully understand every mechanism, the future of scar healing looks increasingly active, precise, and regenerative.